4 Things to Look for When Selecting Provider Credentialing Software

There’s a lot of advice online about how to compare quotes from software vendors. And you’re not imagining things if you feel as if some companies encourage a speedy decision in selecting a provider credentialing software platform. But due diligence is critical because there’s no one-size-fits-all for provider data management. We offer tips you might not have thought of, regardless of whether you’ve been through the vetting process before.
Use the following statistics and insights to help you treat your provider credentialing software choice like the crucial decision it is—for primary source verification, credentialing, and payer enrollment tasks.
The longevity of a software decision
Regret after inking a contract for credentialing or payer enrollment/provider enrollment (PE) software upon realizing it can’t do what you need? A mistake can hinder careers, curb productivity, and negatively affect your organization’s revenue for years to come.
Consider the statistics about how long and often you should plan to be tied to your software choice, based on survey responses of 500+ provider management organizations nationwide:
- 55% have used the same software program for six or more years
- Two-thirds use their credentialing software for more than 50% of their day
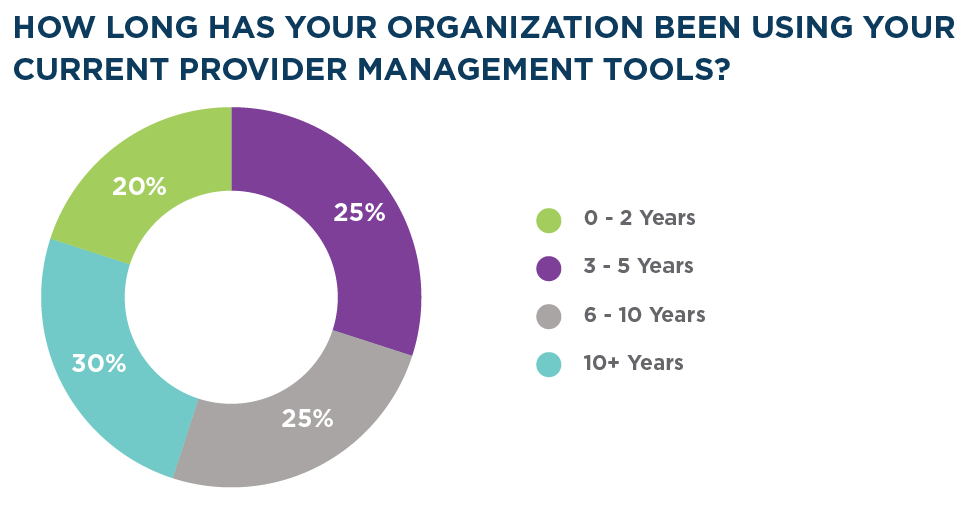
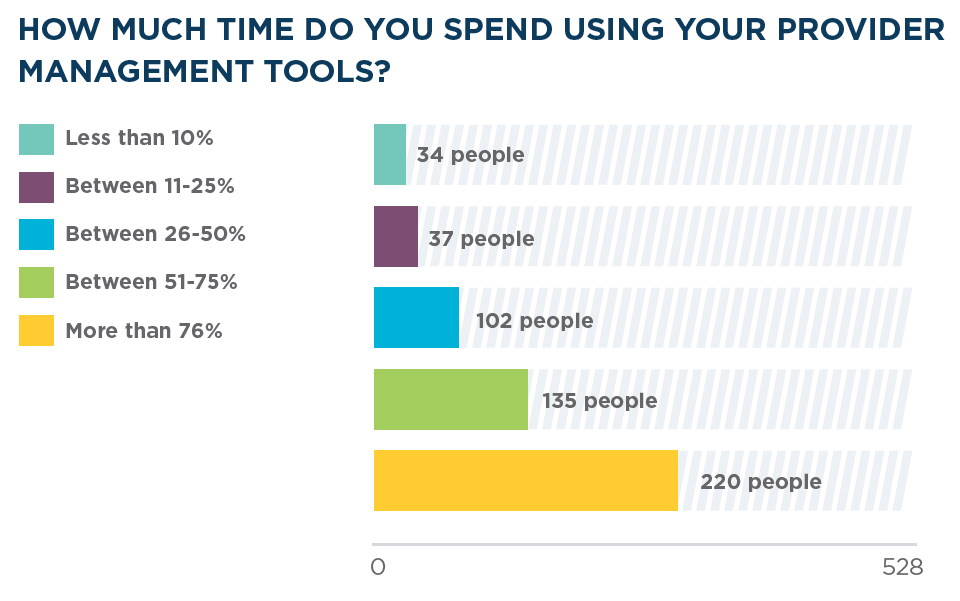
Source: "Industry Insights: Provider Data Management Software," a 2019 symplr survey sent to +10,000 healthcare professionals. Data reflects 528 responses.
Consider these four critical areas as you compare quotes and assess multiple credentialing or PE solutions during your research phase.
1. Price and value
Price is a top consideration because ultimately the budget reigns supreme. But beware if, during the bidding process, a quote comes in significantly lower than others. Price isn't the same as value. An established software vendor will flex slightly on price to win your business. However, if you encounter a solution that’s thousands of dollars less, your red flag (the same one you use during credentialing) should rise. New and alternative software companies haven't discovered a trick allowing them to offer similar tools and service at a significantly lower price than others. The fact is, the offering or the support will not be as robust or evolved. Otherwise, all vendors would cut their price arbitrarily to compete. You get what you pay for; it’s true for paper plates, shoes, and software.
Look for a software partner who does not just offer automation, but one that can also provide an industry-validated best practice approach to implementation and optimization.
Another reason to beware a significantly lower initial price: Often, customers find that once they’re in the door, they’re hit with continuously increasing annual costs. Per-provider or per-facility fees aren’t ideal for organizations experiencing growth.
Last, value’s also reflected in service and implementation costs. What customization and changes exactly will you be able to make on your own in the system, as opposed to paying the vendor to make them? And if 10 hours of implementation are included, for example, ask if that will cover you in full—or whether you should expect to buy more hours based on similar implementations.
2. Ease of use and functionality
Flashy, new, fun. Elements on a dashboard look great in demos. Fast-forward two to six months after integration. That’s about the time when you’ll have had your hands well into the full gamut of functions and reports. What’s behind that colorful user interface?
![]() Custom fields
Custom fields
![]() The ability to self-create and run reports
The ability to self-create and run reports
![]() Web crawlers
Web crawlers
![]() Schedulers that auto-run
Schedulers that auto-run
These are the start of the checklist you should present to each vendor for confirmation of a task’s or function’s inclusion. Identify what’s important to your department, organization, and the future users of the solution.
Functionality is perhaps the hardest thing to gauge when all you have to go on is a demo or two. Keep in mind that an out-of-the-box model is what’s usually demoed initially, but additional conversations must include your users; IT support; and Quality, Enrollment, or Medical Staff department representatives, etc., as appropriate. On the vendor side, don’t just rely on your sales rep. Converse with other vendor personnel—operations, developers, and implementation specialists. Finally, talk to customers of each product to learn from their user experiences.
3. Scalability for long-term plans
If you’re vetting and selecting software, it’s likely that your role gives you access to your organization’s short-, medium-, and long-term goals related to the provider data that the solution will hold. If you’re unsure what the goals are, ask—and share them with the vendor to the extent possible. If the sales or support team from the prospective software company can’t show you how the product can be scaled or configured to meet each of those goals today and down the road via the current or planned future versions, it’s not a good fit.
Regarding functionality in development: Ask when it will be available, how it will work, and whether the vendor will share release notes or connect you with a developer for questions.
Some goals or future plans of your organization may include or affect:
- Provider volume
- Number and type of facilities
- Staff users and their changing roles and responsibilities
- Specific departmental project initiatives.
But beyond those basics, your organization’s goals are unicorns. Every organization grows in response to its own culture, competition in its space and geography, and leadership initiatives. Your credentialing software must change and grow with you.
4. A representative and a partner
If your organization is like others, you’ll have carefully compared at least two solutions by the end of your due diligence process. It’s decision time and the choice might come down to minor differences. That’s a good thing, but the contract step often paralyzes software buyers. Any experienced sales representative will tell you that it’s this phase where most prospective clients go radio silent. However, doing so is a missed opportunity. Read and understand the contract. Use this time to talk to your representative honestly about your concerns and comparison requests.
Perhaps you have naysayers or roadblocks within your organization preventing a final decision. Your sales representative has the ammunition you need in the form of data and talking points to help you move forward and get the tools you need. Treat your sales rep like the partner they may become, and you’ll be surprised by how accommodating they can be if your decision-point differences are small between vendors. Consider, too, that the way you’re treated now generally reflects how your long-term relationship with the company would go.
When you want advice or feedback in credentialing or enrollment, you tap into the advice of veterans who have experience with the content and the community of users. Likewise, it speaks volumes when a vendor has served an industry for a significant number of years. Longevity in any business is not a coincidence.
Everyone in credentialing and payer enrollment is busy and getting busier due to added responsibilities. But don’t fall victim to making a quick decision when you have tools at your disposal to conduct true due diligence and get what you want the first time around.
Learn how symplr can help with your provider data management.